 A pig's heart.
A pig's heart. A pig's heart.
A pig's heart.
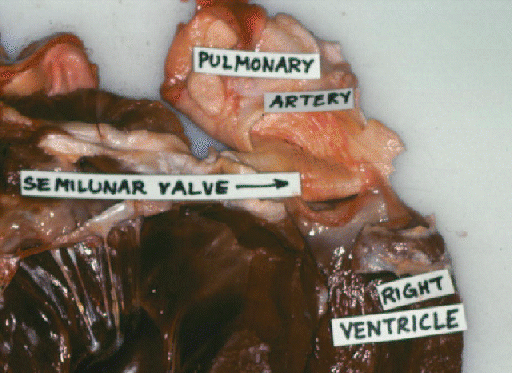 Here are the bovine semilunar valves.
Here are the bovine semilunar valves.
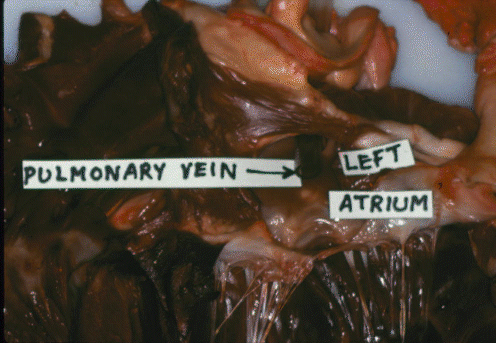 Here is the bovine pulmonary vein.
Here is the bovine pulmonary vein.
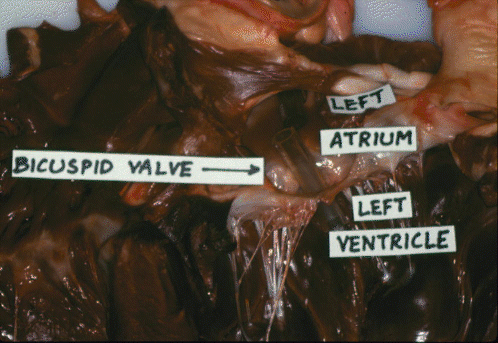 Here is the bovine bicuspid valve.
Here is the bovine bicuspid valve.
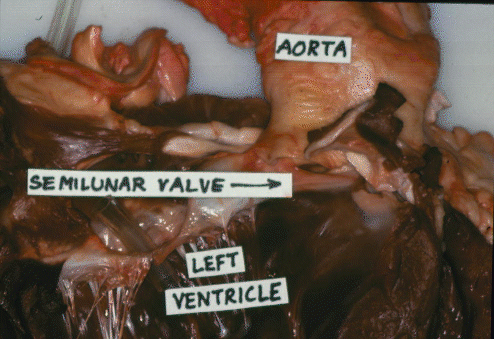 Here is the bovine aorta.
Here is the bovine aorta.
There are three different types of muscle tissue in the body -smooth, cardiac and skeletal (Figure 1-13). Smooth muscle occurs in the digestive and reproductive tracts, cardiac muscle is only found in the heart, while skeletal muscle forms all the meat of the commercial carcass.
Most cardiac muscle cells are mononucleate. They are arranged in rows to form branching fibers, but individual cells are separated by intercalated discs. Cardiac muscles have a striated appearance due to the precise alignment of sliding filaments in their contractile fibrils, but skeletal muscles also are striated.
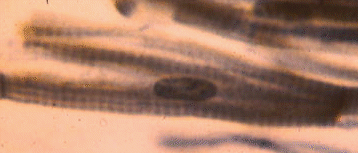 This is a lateral view of a squashed cardiac muscle cell. The nucleus is fairly obvious, as are the transverse striations, but it is difficult to see how this was once part of a branched cardiac muscle fiber.
This is a lateral view of a squashed cardiac muscle cell. The nucleus is fairly obvious, as are the transverse striations, but it is difficult to see how this was once part of a branched cardiac muscle fiber.
 This is a transverse section of a group of cardiac muscle fibers, showing how their nuclei are located centrally in the axis of each fiber.
This is a transverse section of a group of cardiac muscle fibers, showing how their nuclei are located centrally in the axis of each fiber.
Cardiac muscle cells are continuously pumping out sodium ions through their membranes. This causes the inside of the cell to have an electrical charge of approximately -90 mV with respect to the outside of the cell. This is called a resting potential. Extrinsic factors such as electrical activity (ionic movements) in adjacent cells may decrease the resting potential towards zero. When it reaches a value of approximately -65 mV, the threshold potential, the decrease in electrical potential accelerates, and it shoots past the zero value so that for a brief instant (about one tenth of a second) the membrane potential is positive. This sudden reversal of electrical charges is called an action potential. Action potentials are propogated into the interior of cardiac muscle cells by transverse tubules. In each cell, the transverse tubular system is an extensive series of finger-like indentations of the surface membrane.
The arrival of an action potential in the interior of the cardiac muscle cell causes the release of calcium ions from the sarcoplasmic reticulum. The sarcoplasmic reticulum is a series of membrane-bounded vesicles in the interior of the cell. Unlike the transverse tubular system, the sarcoplasmic reticulum does not open to the surface of the muscle cell. Units of the sarcoplasmic reticulum surround the contractile fibrils in the interior of cardiac muscle cells. The sarcoplasmic reticulum sequesters and stores calcium ions, but it releases them again when prompted to do so by the transverse tubular system. Calcium ions activate the system of sliding protein filaments which is responsible for muscle contraction.
The intrinsic rhythm of heart contraction originates from a group of cells at the sinu-atrial node. The membranes of these cells behave as if they had a sodium ion leak. Thus, at regular intervals their resting potentials drop to their threshold values, and they initiate action potentials. Action potentials then spread in a coordinated wave through right and left atria. The atria then contract and pump blood into the ventricles. However, the ventricles also are capable of filling themselves as they expand after pumping out their previous fill of blood. Under normal conditions, atrial contraction contributes to the overall cardiovascular efficiency, but its contribution may become vital when the heart is weakened by disease. In the medial wall of the heart, at the junction between the atria and ventricles, is a sensitive group of cells forming the atrioventricular node. This node is connected to a conduction system called the bundle of His that runs down the medial wall separating left and right ventricles. The atrioventricular node is activated by contraction of the atrial cells, and the bundle of His conducts the action potential wave to the base of the ventricles. From this point, a wave of contraction spreads upwards through the ventricles so that the the blood that has just filled the ventricles is now pumped out of the heart. The intrinsic heart rate is determined by the rate at which the sinu-atrial cells "leak" or depolarize, by the value of their threshold potentials, and by their resting potential. The flow of blood through the heart is directed by the heart valves (Figure 1-8). Mitral and tricuspid valves make a "lub" sound and the semilunar valves make a "dup" sound.
Coordinated electrical activity of cardiac muscle cells generates an electrical signal that may be detected on the surface of the fore flank as an ELECTROCARDIOGRAM(Figure 1-14).
The nervous system also has an effect on heart rate. The thoracic nerve of the sympathetic nervous system releases catecholamines that increase the heart rate (tachycardia) while the vagus nerve of the parasympathetic nervous system releases acetylcholine that slows the heart (bradycardia). The neural regulation of cardiac activity is a reflex response to inputs from blood pressure receptors or baroreceptors, and from chemoreceptors that monitor the concentration of carbon dioxide in the blood. When the heart contracts, it works against the resistance to blood flow created by the peripheral blood vessels in the body tissues. Thus, if the peripheral blood vessels decrease their diameter (vasoconstriction), the blood pressure tends to rise. Conversely, if peripheral blood vessels are dilated (vasodilation), the blood pressure tends to drop.